Assessment of the Adequacy of Manpower, Equipment and Material Resources for the Provision of Primary Mental Health Services in PHC Facilities in Rivers State, Nigeria
Main Article Content
Abstract
Background: To maintain the good mental health of a population, the primary healthcare delivery system must be enhanced to provide mental healthcare services (MHS). This study was thus aimed at assessing the adequacy of manpower, equipment, and material resources for providing mental healthcare services in primary healthcare (PHC) facilities in Rivers State, Nigeria.
Methods: This study employed a descriptive cross-sectional design and was conducted in 123 Model Primary Health Care (MPHC) facilities in Rivers State, Nigeria. The heads of facilities provided responses on the availability of manpower, equipment, and material resources necessary for the provision of MHS. Data were collected using an adapted manpower, equipment, and materials checklist, after which evaluation was performed using laid-down PHC standards to determine the adequacy of the assessed resources.
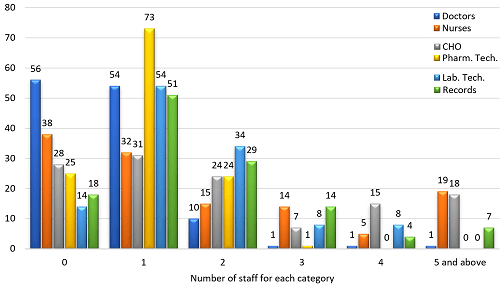
Results: Regarding the manpower working at the health facilities, it was identified that 56 (45.5%) facilities had no doctors and 38 (30.9%) had no nurses, one community health officer (CHO) in 31 (25.2%), among other workers. The various cadres of workers in the PHC facilities were also identified as grossly inadequate. An assessment of equipment and material adequacy, using a 50% cutoff to classify availability as “adequate” or “inadequate”, showed that most facilities (64, 52.0%) experienced inadequacies in these equipment and materials.
Conclusion: The manpower, equipment, and material resources required for the provision of MHS in PHC facilities in Rivers State was found to be inadequate and inequitably distributed. It was thus recommended that the relevant healthcare stakeholders in the State should work to strengthen the capacity of PHC facilities to provide quality MHS to the Rivers populace, thereby improving health outcomes.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
References
- Chuku CN, Obiageli O. Manpower Development and Utilization of Health Care Delivery in Portharcourt Metropolis of Rivers State. ESUT Journal of Social Sciences. 2019, 4(1): 77–88.
- World Health Organisation. Mental Health, 2025. https://www.who.int/news-room/fact-sheets/detail/mental-health-strengthening-our-response
- Votruba N, Thornicroft G. The importance of mental health in the Sustainable Development Goals. BJPsych International. 2015, 12(1): 2-4. https://doi.org/10.1192/s2056474000000027
- Lawal SA, Henderson D, Ogunniyi A. Revisiting the need to strengthen health systems in Africa for better mental health care delivery. The Nigerian Health Journal. 2022, 22(2): 225-243.
- Soroye MO, Oleribe OO, Taylor-Robinson SD. Community Psychiatry Care: An Urgent Need in Nigeria. Journal of Multidisciplinary Healthcare. 2021, Volume 14: 1145-1148. https://doi.org/10.2147/jmdh.s309517
- Jack-Ide IO, Uys LR, Middleton LE. Mental health care policy environment in Rivers State: experiences of mental health nurses providing mental health care services in neuro-psychiatric hospital, Port Harcourt, Nigeria. International Journal of Mental Health Systems. 2013, 7(1). https://doi.org/10.1186/1752-4458-7-8
- Rivers State Ministry of Health. Rivers State Government Strategic Health Development Plan, 2010--2015. 2015, 1–63.
- Afolayan JA, Okpemuza M. Sociocultural Factors Affecting Mental Health Service Delivery in Neuropsychiatric Hospital, Port Harcourt, Rivers State, Nigeria. Nursing Science. 2011, 3(1): 31-40.
- Ofori SN, Adiukwu FN. Screening for Depressive Symptoms among Patients Attending Specialist Medical Outpatient Clinics in a Tertiary Hospital in Southern Nigeria. Psychiatry Journal. 2018, 2018: 1-6. https://doi.org/10.1155/2018/7603580
- Nwaopara U, Stanley P. Prevalence of Depression in Port Harcourt Prison. Journal of Psychiatry. 2015, 18(6). https://doi.org/10.4172/2378-5756.1000340
- National Primary Health Care Development Agency. Minimum standards for Primary Health Care in Nigeria, 2021.
- Keynejad RC, Dua T, Barbui C, et al. WHO Mental Health Gap Action Programme (mhGAP) Intervention Guide: a systematic review of evidence from low and middle-income countries. Evidence Based Mental Health. 2017, 21(1): 30-34. https://doi.org/10.1136/eb-2017-102750
- Scheffler RM. Human resources for mental health: workforce shortages in low- and middle-income countries. Geneva, Switzerland, 2011.
- Anyebe EE, Olisah VO, Garba SN, et al. Barriers to the provision of community-based mental health services at primary healthcare level in northern Nigeria – A mixed methods study. International Journal of Africa Nursing Sciences. 2021, 15: 100376. https://doi.org/10.1016/j.ijans.2021.100376
- Petersen I, Lund C, Bhana A, et al. A task shifting approach to primary mental health care for adults in South Africa: human resource requirements and costs for rural settings. Health Policy and Planning. 2011, 27(1): 42-51. https://doi.org/10.1093/heapol/czr012
- Chingiz Guliev, Zoryana Lebedyn, Alina Frolova, et al. Integrating mental health assessment in primary health care: Challenges, innovations, and economic implications in low-resource settings. International Journal of Science and Research Archive. 2025, 16(1): 763-771. https://doi.org/10.30574/ijsra.2025.16.1.2072
- Oghenerukevwe T, Ameh S, Tella AO. Pattern and Determinants of Depression Among Students Attending Tertiary Institutions in Rivers State, Nigeria. International Journal Of Research and Innovation In Social Science. 2022, 6: 529–535.
- Muhorakeye O, Biracyaza E. Exploring Barriers to Mental Health Services Utilization at Kabutare District Hospital of Rwanda: Perspectives From Patients. Frontiers in Psychology. 2021: 12. https://doi.org/10.3389/fpsyg.2021.638377
- Kuhnt J, Vollmer S. Antenatal care services and its implications for vital and health outcomes of children: evidence from 193 surveys in 69 low-income and middle-income countries. BMJ Open. 2017, 7(11): e017122. https://doi.org/10.1136/bmjopen-2017-017122
- Duara HB, Sylva DG, Binabo TC. An exploratory study of mental health service of families and persons with psychological health issues in the Niger Delta region , Nigeria. African Journal of Nursing and Midwifery. 2015, 2: 149–155.